Artificial intelligence (AI) is rapidly reshaping adult cardiovascular medicine and cardiac surgery, marking a transition from traditional, experience-driven care toward data-driven, predictive, and personalized medicine. This review highlights how AI technologies are now being deployed across the entire perioperative continuum—from preoperative diagnostics to intraoperative assistance and postoperative care—while also addressing the limitations and future directions of the field.
In the preoperative phase, AI has significantly enhanced diagnostic accuracy and risk stratification. Deep learning algorithms applied to electrocardiograms (ECGs) can detect subtle cardiac dysfunction that may not be visible to clinicians. For example, AI models have demonstrated the ability to identify left ventricular dysfunction and predict long-term outcomes using simple ECG data. Similarly, AI-driven imaging tools improve interpretation of echocardiography, CT, and MRI scans by automating segmentation and identifying disease patterns with high precision. These advances allow for earlier detection of disease and more accurate surgical planning.
Risk prediction has also evolved beyond traditional tools such as EuroSCORE II and the STS calculator. Machine learning models can analyze complex, high-dimensional datasets—including labs, imaging, and clinical variables—to generate individualized risk profiles. These models often outperform conventional statistical approaches, particularly in heterogeneous patient populations. Importantly, AI can identify nonlinear relationships and hidden risk patterns, enabling more precise decision-making and personalized surgical strategies.
Surgical planning has been transformed by AI-enabled 3D reconstruction, virtual reality (VR), and augmented reality (AR). Surgeons can now interact with patient-specific anatomical models, rehearse procedures, and anticipate complications before entering the operating room. AI-driven segmentation dramatically reduces the time required to create these models, making advanced planning tools more accessible. These technologies improve surgical confidence, enhance team communication, and may reduce intraoperative uncertainty.
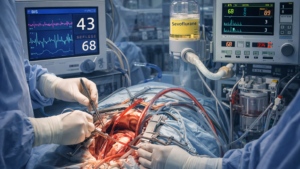
During surgery, AI is increasingly integrated into robotic systems and intraoperative monitoring tools. AI-enhanced robotics improve precision through motion stabilization, tremor reduction, and intelligent instrument tracking. Computer vision algorithms can identify anatomical structures in real time, detect bleeding, and monitor surgical technique. Innovations such as the Hypotension Prediction Index (HPI) allow clinicians to anticipate hemodynamic instability before it occurs, shifting care from reactive to proactive. Early evidence suggests these tools can improve physiologic stability and reduce complications.
Postoperatively, AI plays a critical role in monitoring and early detection of complications. Machine learning models analyze continuous physiologic data and electronic health records to predict events such as acute kidney injury, low cardiac output syndrome, respiratory failure, and sepsis hours before clinical deterioration becomes apparent. Early-warning systems and predictive analytics enable timely intervention, potentially reducing ICU stays and mortality. Additionally, AI-driven remote monitoring systems extend care beyond the hospital, improving follow-up and reducing readmissions.
Despite these advancements, significant challenges remain. Much of the current evidence is based on retrospective studies, with limited prospective validation or randomized trials. Data heterogeneity, variability in clinical workflows, and differences in electronic health record systems can limit model generalizability. Bias in training datasets may lead to unequal performance across different patient populations, raising concerns about fairness and equity. Furthermore, the “black box” nature of many AI models creates challenges in transparency and clinician trust.
Regulatory and ethical considerations also play a critical role in AI adoption. Ensuring data privacy, maintaining model performance over time, and defining liability in AI-assisted decision-making are ongoing concerns. Integration into clinical workflows remains another barrier, as poorly designed systems can lead to alert fatigue or underutilization.
Looking ahead, the future of AI in cardiac surgery is promising. Emerging technologies such as multimodal foundation models and digital twins aim to integrate imaging, physiologic data, and genomics into comprehensive patient-specific simulations. These tools could allow surgeons to predict outcomes, optimize procedures, and personalize treatment strategies with unprecedented accuracy. Additionally, advancements in semi-autonomous robotics and AI-enabled hybrid operating rooms may further enhance precision and efficiency.
In conclusion, AI is transitioning from experimental innovation to real-world clinical application in adult cardiac surgery. While challenges remain, its ability to improve diagnostics, enhance surgical planning, and predict complications positions AI as a transformative force in cardiovascular care. With continued validation, ethical oversight, and thoughtful implementation, AI has the potential to significantly improve patient outcomes and redefine the future of cardiac surgery.